Why Systems-Level Changes Are Needed to Address Health Worker Well-Being

From the earliest days of the COVID-19 pandemic, it was clear that health workers across specialties, disciplines, and care settings were not going to be okay. Having limped into a novel global health crisis—after decades of alarm bells observing that clinicians were burning out at an accelerated rate—health workers (defined broadly by the Surgeon General as “all the people engaged in work to protect and improve the health of individuals, communities, and populations, including those who assist in operating health care facilities”) put their lives on the line in every way. The worst of the pandemic lasted far longer than anyone could have expected. And the declared “end” of the public health emergency in May 2023 did not magically erase COVID-19 or its consequences.
Recognizing the threat to health worker well-being, CAPC (and many, many other organizations across the country) went all in on developing resources to address emotional, social, moral, and psychological suffering. On came a word salad of concepts to describe what was happening in the heads and hearts of frontline clinicians: stress, anxiety, burnout, moral distress, moral injury, empathic strain, compassion fatigue, ennui, languishing, “my brain is melting,” etc. We offered webinars on building resilience and managing uncertainty, promoted centering techniques developed by psychologists and other experts, and wrote blogs on just getting through. We launched the Breaking Point podcast and virtual debriefing sessions. We shared resources about how palliative care teams could leverage this moment to demonstrate their institutional value, such as integrating themselves into organizational wellness initiatives or leading their own debriefings. CAPC packaged it into a bundle called “Emotional PPE,” mirroring the language of physical personal protective equipment (PPE) to underscore the urgency of attending to health workers’ emotional health.
It was not enough.
Three years into the pandemic, Dr. Don Berwick asked us to consider the following at a National Academy of Medicine (NAM) event:
"Imagine a [health care leader], who gets in her car in the morning to drive to work, [her mind] already spinning about everything she is leading. Stuff she wasn’t necessarily prepared for when she signed on to become a leader in a health care organization. Climate activists are demanding that the hospital pledge to decarbonize care. Recently published data on racial disparities in local care, access, and outcomes have brought anger about inequity to the boiling point in her community. The pandemic may be waning at last, but it has left a wake of exhaustion and the staff resignations are at an unprecedented level. The acute shortage of nursing has forced units to close, and a lot of nurses have left the hospital to seek better working conditions by becoming traveling nurses, with the paradoxical effect that a hospital has to hire back—in temporary roles at higher costs—the same people who have recently resigned from full-time work. There has been a recent newspaper story about a surgery gone wrong and we have this whole re-ignition of concerns about patient safety. Governments at all levels are trying to adjust the lessons of the pandemic into plans for participation of public health and preparedness for the next pandemic, and it’s on her desk to do that. Primary care clinicians and community groups are making louder and louder claims about the importance of social determinants of health, and they are asking the hospital to respond by managing or funding food clinics, and housing supports, and more responsive mental health services, in-home supports for isolated and frail elders. It is really hard to be a leader in health care today. It probably always has—but this list is astounding."
Our health care system is decimated. And one of the most significant reasons for this is that our country has abused its health workforce for too long. Overwhelming patient volume, burdensome documentation requirements, complex policies, rapidly changing technology, public health denialism, increased risk of encountering violence, facility closures, and negligible concern for work-life balance (among other things) have led to an exodus of clinicians who are saying “enough.” Many who remain exist somewhere on a continuum from quietly struggling, all the way to leading efforts to demand more humane and sustainable work conditions.

None of the circumstances listed above will be resolved by deep breathing. Health workers have already demonstrated significant amounts of resilience. The burden of responsibility is not on the individual clinician. Systems-level changes are needed to make the work of caring for patients safer, healthier, better compensated, and ultimately more sustainable. These efforts must include tending to the workforce of today, and growing the pipeline of the workforce tomorrow. And doing so will require advocacy at the organizational, state, and federal levels.
Systems-level changes are needed to make the work of caring for patients safer, healthier, better compensated, and ultimately more sustainable.
Recent National Activities
The good news—if you can call it that—is that the health care workforce crisis is so large that policymakers have taken notice. In February and March 2023, the U.S. Senate Committee on Health, Education, Labor & Pensions (HELP) held a full committee hearing and issued a request for information in which they acknowledged alarming health care workforce shortages and sought information on the causes and potential legislative solutions. During this hearing, Senator Tammy Baldwin highlighted how Palliative Care and Hospice Education and Training Act (PCHETA, S. 2243 in the 118th Congress) could address each aspect of the health care workforce pipeline for palliative care. Meanwhile, states have introduced promising programs to address provider wellbeing, reduce administrative burdens, and ensure provider safety (among other topics). Notably, Illinois introduced HB3571 which, if passed, would create a Community Hospice and Palliative Care Professional Loan Repayment Program.
Two other notable national initiatives have launched that look at systems-level causes and solutions for the issues challenging our health care workforce:
1) Addressing Health Worker Burnout: The U.S. Surgeon General’s Advisory on Building a Thriving Health Workforce
In May 2022, US Surgeon General Dr. Vivek Murthy published an Advisory to draw attention to the public health crisis presented by a depleted workforce. This report clearly describes how the U.S. health care ‘system’ has betrayed our health care workers (see Figure 1 above), and the current and future consequences of these failures—including irreconcilable harm (physical, mental, and emotional) to our health care workers, leading to illness and even loss of life; and further extreme provider shortages that will limit access to routine and emergency care for millions of people. What this report does particularly well is lay out recommendations tailored to actors at all levels, recognizing that meaningful change will only occur if every stakeholder takes action. Examples include (but are not limited to):
- Health care organizations must assess, measure, respond to, and intervene to prevent occupational distress and burnout; show health workers how much they are valued through transparent communication, living competitive wages and affordable health coverage, and family-friendly policies; review and revise policies to ensure health workers are not deterred from seeking appropriate care for physical health, mental health, and/or substance use challenges; and combat bias, racism, and discrimination, as well as health misinformation, in the workplace.
- Federal, state, local, and tribal governments must invest in evidence-based practices, plans, and partnerships that ensure the health, safety, and well-being of health workers including paid leave and rest time policies; develop and invest in reimbursement models that are aligned with the goals of high-quality, person-centered care; reduce administrative burdens (a consistent theme throughout this document) contributing to health worker burnout—particularly clarifying regulations and documentation requirements; and recruit, expand, and retain a diverse health care and public health workforce to meet current and future health challenges.
- Health insurers and payers must support the quality and quantity of time that health workers can spend with patients through alternative reimbursement models; reduce administrative burden posed by prior authorization requests and other documentation and reporting requirements; and ensure that clinical care, preventive services, quality mental health, and substance use care are available to health workers.
- Health care technology companies must design technology to serve the needs of health workers, care teams, and patients across the continuum of care by making electronic health records more accessible and efficient (including designing platforms with interoperability in mind); strengthen the integration of data across platforms and health sectors, including adopting a standard format for how health data is stored and exchanged; and co-designing telemedicine and virtual care services in partnership with end-users including health workers, patient populations, and families.
- Academic institutions, clinical training programs, and accreditation bodies must protect and preserve the precious resource that is health worker students and trainees (who are noted as particularly vulnerable to burnout) by prioritizing, assessing, and supporting learner well-being; acknowledging and correcting the hidden curriculum within health professional education; promoting access to mental health and substance use care; promoting inclusion and diversity; and fostering peer connectedness.
The final action sections are dedicated to family members, friends and communities; health care workers; and research. And while these recommendations are decidedly important, positioning the family and workers at the end of the Advisory implicitly relieves some of the pressure on these stakeholders to solve issues that are not of their own making.

2) National Plan for Workforce Well-Being
In October 2022, the NAM Action Collaborative on Clinician Well-Being and Resilience published its National Plan for Health Workforce Well-Being. The launch event included introductory remarks from U.S. Representative Ami Bera (D-CA), U.S. Representative David P. Joyce (R-OH), and U.S. Senator Tim Kaine (D-VA), as well as influential leaders across the government, private, and non-profit sectors. Building off the framework created in the 2019 NAM Report Taking Action Against Clinician Burnout, this plan included the following seven priority areas:
- Create and Sustain Positive Work and Learning Environments and Culture
- Invest in Measurement, Assessment, Strategies, and Research
- Support Mental Health and Reduce Stigma
- Address Compliance, Regulatory, and Policy Barriers for Daily Work
- Engage Effective Technology Tools
- Institutionalize Well-Being as a Long-Term Value
- Recruit and Retain a Diverse and Inclusive Health Workforce
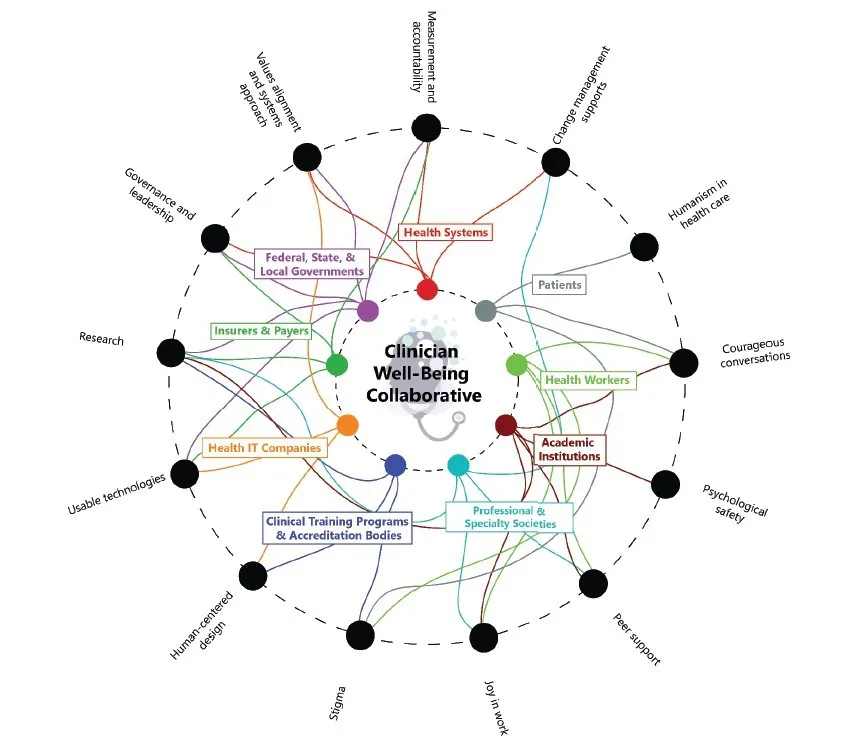
Again, this report was developed with the collaboration of actors across sectors (see Figure 3), and it explicitly names which of these actors must take action within a priority and what action they must take. Beyond that, it provides relevant tools to take those actions.
The most significant shortcoming of these two initiatives is that they do not have the rule of law behind their recommendations, nor do they provide funding to support action. However, the credibility of these organizations, paired with the commitment of important stakeholders who were at these tables and some (although not yet enough) federal funding targeted towards addressing these issues provides an important place to start. The next step is to leverage the recommendations from these initiatives to respond to opportunities such as the HELP Committee request for information previously discussed; and for health worker leaders to identify and implement recommendations that are targeted towards their locus of control.
What Team Leaders Can Do
The work of systems-level advocacy is long and, frankly, can be discouraging. In the meantime, there are things that team leaders can do to address some of the structural issues that erode health worker well-being. Looking specifically to palliative care, CAPC’s toolkits on Emotional PPE and Leadership Skills in Palliative Care have bundles on developing leadership skills to support team cohesion and wellness, cultivating psychologically safe environments for health care workers, and identifying creative solutions to address personal circumstances that impact work (e.g., caregiving). The Institute for Healthcare Improvement (IHI) offers resources on Joy in Work. And CAPC’s leadership offerings will continue to include considerations for emotional PPE as well as health equity.
In the meantime, there are things that team leaders can do to address some of the structural issues that erode health worker well-being.
Depending on your capacity, it may be worth exploring the initiatives above to learn more about opportunities for organizational and policy change. While self- and team- care are your primary obligations, these larger system efforts need champions to ensure that preserving our health workforce remains front and center.
Conclusion
These continue to be challenging times. Our workforce is tired and diminished in numbers. There is no cavalry coming, no magical fix that will immediately resolve the longstanding and systemic issues discussed in this article. These are realities that we must acknowledge as we all make the daily decision about whether or not to remain in health care.
CAPC will continue to offer streamlined resources to support individual clinicians who are looking for a little extra help with their emotional needs. We do this because there are many evidence-based strategies to bolster coping. Attendees of our open-access debriefings report that they provide invaluable support—both in helping to normalize their experiences and emotions, and facilitating peer-to-peer sharing that can generate solutions to structural issues. We also offer Virtual Office Hours for those interested in leading debriefings in their own organizations. Finally, the upcoming C-TAC-CAPC Leadership Summit (October 23-24, 2023) will focus heavily on workforce challenges and strategies, and include the session “Practice Strategies to Support Team Well-Being” with Drs. Michelle Owens and Elizabeth Holman.
As we state in the Emotional PPE toolkit, CAPC firmly believes that it is the responsibility of organization, state, and federal leaders to create a more supportive and sustainable environment for health care clinicians.
But as Dr. Berwick noted as he finished in his remarks at the NAM event, any change efforts cannot be another “problem” to drop on the desk of the health worker or team leader—solutions must be crafted using a contextual approach. As we state in the Emotional PPE toolkit, CAPC firmly believes that it is the responsibility of organization, state, and federal leaders to create a more supportive and sustainable environment for health care clinicians. Our focus moving forward will be identifying and/or developing resources that leaders can use to change structures—be it through cultivating safety within teams, advancing institutional change, and/or pursuing supportive public policy. At the same time, CAPC will continue to focus the attention of health care organizations, payers, and policymakers on needs of our workforce, and to work with coalitions such as the National Coalition for Hospice and Palliative Care, the Patient Quality of Life Coalition, and the Coalition to Transform Advanced Care to advocate for change.

Be the first to read articles from the field (and beyond), access new resources, and register for upcoming events.
Edited by Melissa Scholl. Clinical review by Andrew Esch, MD, MBA.
