How States Are Using CAPC’s Serious Illness Scorecard to Improve Care

Recognizing the growth of palliative care in the U.S., CAPC launched the Serious Illness Scorecard (Scorecard) in December 2024 to serve as a roadmap and advocacy tool for state palliative care champions. The Scorecard built on the legacy of the previous State-by-State Report Card (from CAPC and the National Palliative Care Research Center) by establishing a new methodology to assess state capacity; specifically, going from one measure (the proportion of hospitals with 50 or more beds reporting a specialty palliative care program) to ten measures across five domains.
Following a successful national launch, CAPC’s Health Care Transformation (HCT) team recognized that palliative care champions at the state level might benefit from additional support to review and contextualize Scorecard findings. With the “Scorecard Roadshow” (Roadshow), we developed customized presentations for state champions—delivered virtually and in-person—to help them better use the Scorecard for strategic planning and advocacy.
This blog post recaps Roadshow highlights, including themes from the state presentations; examples of how state champions are using the information; and next steps for the Scorecard.
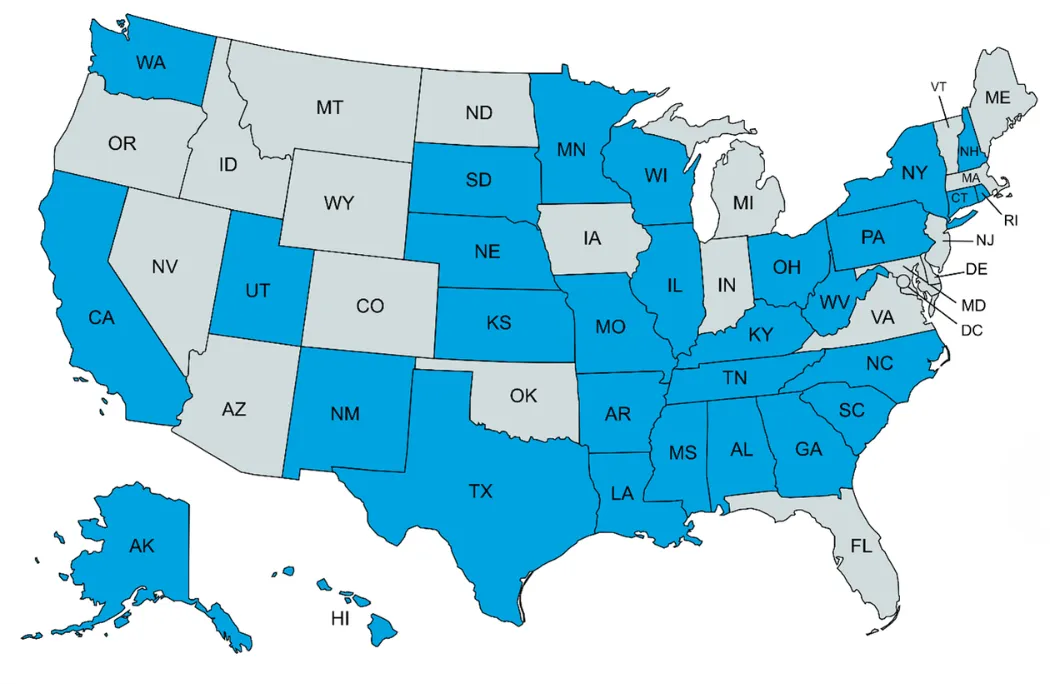
The Scorecard Roadshow
As of December 31, 2025, the team delivered 34 presentations across 30 states (see Figure 1, above). Audiences included state palliative care advisory councils and coalitions, policymakers, collaboratives, and anyone else who is actively involved in advancing palliative care or serious illness-related initiatives in their state. Presentation topics included:
- National landscape of serious illness, including workforce, access to services, and equity considerations
- Explanation of the measures and data sources used to derive state ratings (see Figure 2)
- In-depth exploration of how the state performed on each measure
- Overview of how all states fared nationally on each measure, and customized charts to place the individual state’s performance into context
- Discussion of possible activities the state could pursue, based on actions taken in other states, and how to use the Scorecard to prioritize efforts
- Customized language to most effectively message Scorecard performance to state decision-makers
- Additional free resources, including updated individual state reports, CAPC open access webinars, the patient- and family-facing website Get Palliative Care, and the State Palliative Care Forum for online conversation among state champions.
Scorecard Roadshow Highlights
While each presentation had unique elements based on the state’s rating, the following highlights (both highs and lows) were notable for their inclusion in almost every discussion.
As the field of palliative care matures, the story we tell must be more sophisticated.
This was the primary rationale for how the Scorecard was designed. In the four editions of the State-by-State Report Card between 2006 and 2019, inpatient palliative care access grew dramatically and began to level off. At the same time, programs expanded to provide palliative care services in the community. The broader health care system continued to adopt palliative care principles and practices. And the Report Card was no longer an accurate reflection of all the ways palliative care champions were improving care for people living with serious illness. Reflecting on how far the field of palliative care has come in a short time is something to celebrate.
Reflecting on how far the field of palliative care has come in a short time is something to celebrate.
The Scorecard rates each state’s capacity to advance initiatives to improve the care of people living with serious illness.
A common misconception is that the Scorecard only focuses on palliative care. But CAPC recognizes that quality of life for people with serious illness, and their caregivers, depends on several factors that go beyond specialty palliative care availability. This is why the new domains reflect basic education in palliative care for non-palliative care clinicians in the state, as well as state legislation and programs that provide functional and caregiver supports that are so essential to families facing serious illness.
Scorecard measures were selected to emphasize that palliative care is appropriate across the lifespan.
Variables on expanded payment for specialty palliative care and the existence of a state palliative care coalition include both adult and pediatric initiatives; one variable specifically focuses on whether a state offers extra services for families of children living with serious illness, such as sibling counseling or home modifications. While more information is needed to adequately characterize the experiences of these children and their families, it was critical to CAPC that the Scorecard illustrate that palliative care must also be available for neonates, perinates, infants, children, adolescents, and young adults in need.
Despite expanding its scope, the Scorecard has limitations.
Gaps in data collection in the field mean that there are gaps in Scorecard information as well. The Scorecard does not include the location of community-based palliative care services, nor does it calculate the proportion of people with serious illness in a state that receive palliative care. The first (2024) edition of the Scorecard analyzes state capacity at the level of a palliative care program, though CAPC does not have data to evaluate the structure or quality of palliative care services available. CAPC and other leaders in the field are developing long-term strategies to address these gaps, and we aim for future versions of the Scorecard to include even more comprehensive information.
In the meantime, if you have not already done so, please make sure that your programs are listed (or nudge your colleagues to list their programs) in the Palliative Care Provider Directory; and keep an eye out for the Palliative Pulse. CAPC’s data collection efforts cross-pollinate our various quality improvement and advocacy activities more than you might realize!
Palliative care leaders are trying to improve care in a challenging health care landscape.
Attendees at several presentations specifically mentioned that general challenges in U.S. health care—staffing shortages, financial pressures, and federal policy shifts—are barriers to advancing palliative care. The Scorecard includes sample activities from states, compiled over the last decade-plus, to provide guidance for states seeking to make progress despite real obstacles.
The Scorecard is meant to support palliative care champions.
Without exception, Roadshow attendees do tremendous work to improve quality of life for people living with serious illness. They volunteer their time to participate in state-level efforts, often with no budget or recognition. CAPC designed the Scorecard and individual state reports to reduce the opportunity cost of collecting data or planning new initiatives. Therefore, we encourage champions to leverage any parts of the Scorecard and tailor messaging in whatever ways advance their efforts. CAPC can provide assistance as needed.
QI Project: Recognizing Puerto Rico
CAPC was unable to include the U.S. territories in the Scorecard due to insufficient data. Over the course of the Roadshow, we heard from a palliative care champion who explained that creating a Puerto Rican individual state report—even with data gaps—would make a statement on the need for its inclusion in future health data. In response, we launched the Puerto Rico report in summer 2025, which enabled new conversations to begin in the territory. We look forward to continued engagement on how the Scorecard can be used in this case and, more broadly, to increase equitable access to care for all people living with serious illness.
How States are Using the Scorecard and Roadshow Presentations
CAPC surveyed state champions (21 responses from 19 states) to better understand how they are using the Scorecard. We are inspired by what we heard:
Mobilize action and strengthen statewide collaboration around palliative care.
Respondents reported forming or joining groups specifically aimed at identifying gaps in care and prioritizing strategies to improve their state standings. Several are using the Scorecard to drive organizational planning and strategic priorities.
The South Carolina Coalition for the Care of the Seriously Ill (SCCSI) formed a Scorecard workgroup—comprised of health systems, community-based organizations, payers, and provider entities—with the goal of being in the “Top 20” in the next Scorecard. SCCSI’s first quality improvement project focuses on improving the primary palliative care skills of clinicians across the state through completion of CAPC courses. Activities have included surveying current CAPC member organizations about how they are using clinical training and planning strategies to increase usage through communications efforts to boost awareness.
Bolster ongoing efforts to increase palliative care access.
Champions from Texas specifically shared that they would continue working with state leadership to create a new Supportive Palliative Care benefit for Medicaid recipients. Similarly, attendees from states such as Minnesota and Maine mentioned incorporating the Scorecard into their ongoing efforts to establish Medicaid benefits for community-based palliative care.
Educate and engage external audiences.
Organizations from many states have shared their state Scorecard publicly, referenced the Scorecard in policy conversations, and incorporated the metrics into publications such as annual reports or official documents. For example, New York is planning to use an indicator from the Scorecard (“Count of State’s Certified Hospice and Palliative Care Professionals per 100,000 population”) in its state cancer plan.
Next Steps and Final Thoughts
The Scorecard has become both a strategic planning tool and an organizing framework for state-level progress, dialogue, and accountability. Throughout the Roadshow, we have collected feedback on potential improvements for the next Scorecard, planned for a 2027 release.
In the meantime, if your state has not hosted a Roadshow presentation and would like one, please request one. Please also participate in CAPC data collection efforts, such as the Palliative Care Provider Directory, so we can adequately track palliative care availability in your state.

Be the first to read articles from the field (and beyond), access new resources, and register for upcoming events.
Subscribe

